Avoiding Fatal Blood Clots on Long-Haul Flights
Blood clots are a serious risk for travelers, particularly during and following a long-haul flight. TPG Contributor Christine Cantera speaks to a physician to determine which steps you should take to stay healthy while on the road.
Health issues that arise from traveling have long been a worry for frequent flyers, so we wanted to let our readers know more about pulmonary emboli — otherwise known as blood clots — and offer some preventive advice.
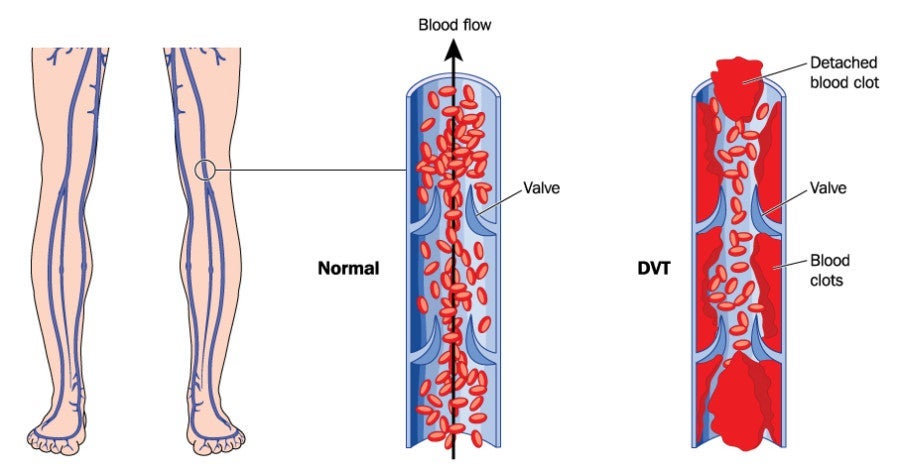
According to the UpToDate® evidence-based clinical decision support resource, deep vein thrombosis (DVT) is the most common type of thrombosis, occurring in the "deep veins" in the legs, thighs or pelvis. If a part or all of the blood clot in the vein breaks off, it can travel through the venous system; this is called an embolus. If the embolus lodges in the lung, it is called pulmonary embolism (PE), a serious condition that leads to over 50,000 deaths a year in the United States. In most cases, PE is caused when part of a DVT breaks off and lodges in the lung.
We asked Dr. John Silbert, a San Diego-based family practitioner for more than 30 years who has cared for many patients with DVT and pulmonary emboli, if he could shed some light on exactly how these conditions happen, and if they can be prevented. (Full disclosure: Dr. Silbert is the father of TPG Copy Editor/Contributor Sarah Silbert.)
"Older people are at higher risk, but younger people are also affected," explains Dr. Silbert. "Most of the time, DVT and pulmonary emboli are acquired conditions, though family history and genetic inheritance often contribute." In fact, Silbert emphasized that they're often related to a patient's personal medical history.
Specifically, a high percentage of DVT and PE cases are associated with the person having been hospitalized within the previous three months. People who are at particular risk include those who've had recent surgery or trauma; are obese; smoke; have cancer; have heart problems; have other chronic diseases including collagen-vascular disease and myeloproliferative disease; women who are pregnant or have been recently pregnant, taking hormone replacement therapies, or on birth control pills; and anyone with kidney disease. Genetic problems can include several disorders related to coagulation, including Factor V Leiden, deficiencies of natural proteins that prevent clotting (e.g., antithrombin, protein C or protein S).

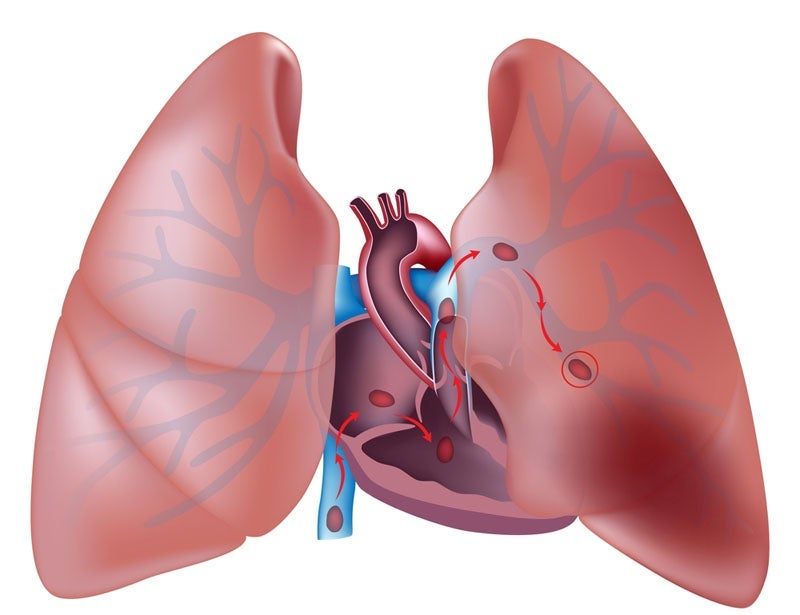
"The key is having the diagnosis of DVT made early enough that treatment can be started to prevent pulmonary embolism from occurring. PE will occur in about 50% of untreated people, usually within days or weeks of the DVT. If it goes untreated there is an overall mortality rate from PE of up to 30%, but much lower when treated. The worst thing that can happen is that you don't get to the clot in time and it travels to the lung", Dr. Silbert explained."DVT and pulmonary emboli have less to do with frequent travel and more to do with the person's health and habits and what was happening within a few months before traveling. The real sorrow is that so many potentially treatable DVT and pulmonary emboli still go undetected."
On that note, all travelers should consider the following recommendations for flights longer than six hours:
- Stand up and walk around every hour or two
- Wear loose-fitting, comfortable clothing
- Flex and extend the ankles and knees periodically, avoid crossing the legs, and change positions frequently while seated
- Consider wearing knee-high compression stockings
- Avoid medications (e.g., sedatives, sleeping pills) or alcohol, which could impair your ability to get up and move around
Be sure to stay aware and listen to your body, and especially if you've been treated for any kind of illness within three months of your journey, follow these instructions to the letter — and above all, travel safe.
Update: Emergency physician Alan Cherney wrote in to share symptoms of DVT and PE. If you experience any of the symptoms below, seek medical assistance immediately.
Signs and symptoms of DVT include pain in the lower extremity, often the calf; redness of the lower extremity; swelling of the calf or lower extremity; difficulty ambulating on the affected lower extremity; swelling of the superficial veins. Signs and symptoms of a PE include chest pain or discomfort; shortness of breath at rest or on exertion; pain with deep inspiration/breathing; palpitations or rapid heart rate; sudden loss of consciousness; coughing up blood; fatigue.
TPG featured card
at American Express's secure site
Terms & restrictions apply. See rates & fees.
| 4X | Earn 4X Membership Rewards® points per dollar spent on purchases at restaurants worldwide, on up to $50,000 in purchases per calendar year, then 1X points for the rest of the year. |
| 4X | Earn 4X Membership Rewards® points per dollar spent at US supermarkets, on up to $25,000 in purchases per calendar year, then 1X points for the rest of the year. |
| 5X | New! Earn 5X Membership Rewards® points on prepaid hotel stays booked through AmexTravel.com or the Amex Travel App. |
| 3X | Earn 3X Membership Rewards® points on flights booked through AmexTravel.com, the Amex Travel App, or purchased directly from airlines. |
| 2X | Earn 2X Membership Rewards® points on prepaid car rentals booked through AmexTravel.com or the Amex Travel App and cruises booked and paid through AmexTravel.com. |
| 1X | Earn 1X Membership Rewards® point per dollar spent on all other eligible purchases. |
Pros
- Valuable dining and food-related credits
- Flexible rewards with airline and hotel transfer partners
- Multiple travel and purchase protections
- No foreign transaction fees
- Access to Amex Offers for additional savings (enrollment required)
Cons
- Not as useful for those living outside the U.S.
- Some may have trouble using Uber and other dining credits
- You may be eligible for as high as 100,000 Membership Rewards® Points after you spend $8,000 in eligible purchases on your new Card in your first 6 months of Card Membership. Welcome offers vary and you may not be eligible for an offer. Apply to know if you’re approved and find out your exact welcome offer amount – all with no credit score impact. If you’re approved and choose to accept the Card, your score may be impacted.
- Earn 4X Membership Rewards® points per dollar spent on purchases at restaurants worldwide, on up to $50,000 in purchases per calendar year, then 1X points for the rest of the year.
- Earn 4X Membership Rewards® points per dollar spent at US supermarkets, on up to $25,000 in purchases per calendar year, then 1X points for the rest of the year.
- New! Earn 5X Membership Rewards® points on prepaid hotel stays booked through AmexTravel.com or the Amex Travel App.
- Earn 3X Membership Rewards® points on flights booked through AmexTravel.com, the Amex Travel App, or purchased directly from airlines.
- Earn 2X Membership Rewards® points on prepaid car rentals booked through AmexTravel.com or the Amex Travel App and cruises booked and paid through AmexTravel.com.
- Earn 1X Membership Rewards® point per dollar spent on all other eligible purchases.
- Pay It® lets you tap in the American Express® App to quickly pay for small purchase amounts throughout the month and still earn rewards the way you usually do. Plan It® gives you the option to split up big purchases into equal monthly payments with a fixed fee. You’ll know upfront exactly how much you’ll pay.
- Updated! $120 Dining Credit: Earn up to a total of $10 in statement credits monthly when you pay with the Gold Card at Grubhub (including Seamless), Buffalo Wild Wings, Five Guys, The Cheesecake Factory, and Wonder. This can be an annual savings of up to $120. Enrollment required.
- $100 Resy Credit: Get up to $100 in statement credits each calendar year at over 10,000 qualifying U.S. Resy restaurants after you pay for eligible purchases with the American Express® Gold Card. That’s up to $50 in statement credits semi-annually. Enrollment required.
- $84 Dunkin' Credit: Earn up to $7 in monthly statement credits after you pay with the American Express® Gold Card at U.S. Dunkin’ locations. Enrollment required.
- $120 Uber Cash on Gold: Enjoy up to $120 in Uber Cash annually with your Gold Card. Just add your Card to your Uber account and you'll get $10 in Uber Cash each month to use on orders and rides in the U.S. when you select an Amex Card for your transaction.
- New! As an American Express® Gold Card Member, you can enjoy complimentary Hertz Five Star® Status. Enjoy benefits like skipping the counter at select locations, adding an additional driver at no additional cost*, and vehicle upgrades**. Benefit enrollment and Hertz Gold+ registration are required. *Additional drivers must meet standard rental qualifications and must be a spouse or domestic partner to qualify as complimentary. Other additional drivers subject to fees. **Benefits are subject to availability and vary by location. Additional Hertz program Terms and Conditions including age restrictions apply.
- Take advantage of a $100 credit towards eligible charges* at over 1,300 upscale hotels worldwide when you book The Hotel Collection through AmexTravel.com or the Amex Travel App **. *Eligible charges vary by property. **The Hotel Collection requires a two-night minimum stay.
- Book your travel through the Amex Travel App with added peace of mind – backed by American Express® service and support. Only for American Express® Card Members.
- Whenever you need us, we're here. Our Member Services team will ensure you are taken care of. From lost Card replacement to statement questions, we are available to help 24/7.
- No Foreign Transaction Fees.
- Annual Fee is $325.
- Terms Apply.

